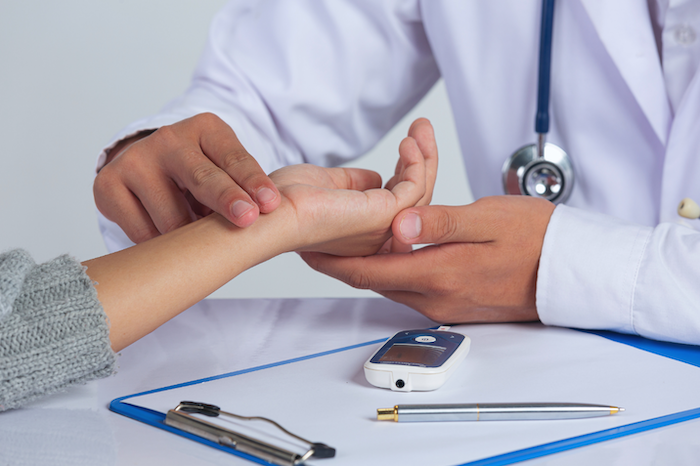
Accidental medical injuries are always sad. Medical malpractice claims based on a doctor’s incorrect diagnosis or failure to recognize a severe illness or condition are especially tragic. A wrong diagnosis or a failure to diagnose will inevitably delay the provision of the necessary care and therapy. This can frequently mean the difference between a person’s life and mortality, between curing their illness and having them pass away. And in some cases, if the proper diagnosis had been made sooner, these accidents would have been avoidable.
When Does Failure to Diagnose Happen?
Failure to identify happens when a doctor misdiagnoses a patient’s illness. Medical mistakes certainly contribute to an even more significant number of injuries. With claimants getting an average settlement of more than $714,000, Chicago has one of the country’s highest average malpractice settlement amounts. According to a ten-year study, Illinois paid over $180 million in medical malpractice cases. Chicago medical malpractice lawyers can defend your interests and assist you in obtaining just compensation—not some paltry settlement meant to appease you.
1. Inexperience and Overconfidence
Diagnostic mistakes can occasionally be the result of novice medical staff. For instance, a practitioner might misdiagnose a patient if they lack the expertise to identify the symptoms of a particular illness. A medical practitioner may also err in their diagnosis if they lack the expertise to:
-
- Know when to perform specific medical tests, or
- Understand how to interpret test findings properly
In other instances, overconfident medical staff members make diagnosis mistakes. For instance, even if a doctor is confident that they are aware of the signs, they may still misdiagnose the patient if they don’t notice them. A doctor may make a diagnostic error if they are overconfident and disregard changes in a patient’s symptoms.
2. Personal Bias
Some patients have a stronger emotional connection with their doctor than others. Although this is understandable, a relationship between a practitioner and a patient may result in the patient receiving inadequate or excessive care. Physicians must adhere to best diagnosis practices to prevent mistakes regardless of the patient they are working with.
3. Insufficient Time with Patients
Studies show physicians only spend around twenty minutes with each patient during appointments. Unfortunately, less than twenty minutes is insufficient for a doctor to fully discuss a patient’s symptoms, thoroughly understand the patient’s medical history, examine the patient’s test findings, and arrive at a diagnosis. Diagnostic blunders are frequently the product of insufficient patient interaction.
4. Not Enough Follow-Up
Patients typically visit various physicians. For instance, if a patient switches insurance, they might visit one specialist before seeing someone else. In other instances, physicians give their patients the duty of following up independently. A patient may suffer the adverse effects of a diagnostic error if a new doctor is not followed up with or if they do not let their doctor know about changes in their state.
5. Insufficient Diagnostic Testing
More than one diagnostic test may be required to depict a patient’s health and identify specific conditions accurately. Healthcare workers may endanger the patient’s life if they do not suggest the appropriate test. Failure to plan the necessary diagnostic tests may result in a lack of understanding of the symptoms. It is a dangerous disease that endangers the patients’ health.
Diagnostic research may be limited when a patient’s insurance coverage is limited. Physicians’ inexperience and arrogance occasionally lead to a lack of diagnostic research.
6. Insufficient Flow of Information
In any healthcare environment, information flow is essential, particularly between various service areas. When patients are transferred to another facility or released from one department to another, the required information does not follow them. This is known as insufficient information flow. Problems with inadequate information movement include those listed below:
-
- The absence of critical knowledge when it was necessary to inform prescribing choices.
- Inadequate dissemination of test findings.
- Medication orders for the transfer of treatment are poorly coordinated.
Bottomline
The cause of the diagnostic error is often multi-factorial, and it could be a result of cognitive errors, which are mistakes in the doctor’s thought process, perhaps because they are rushed; system errors, for example, because of a lack of communication, as a result of which an abnormal lab result is overlooked; and a combination of both. Radiology, geriatrics, and emergency medicine are just a few disciplines more frequently linked to a diagnostic error than others.
Read More:
Preventive lifelong changes to reduce the risk of breast cancer